
These are techniques are used to extract sperm if a man does not have sperm in his semen (azoospermia). Normally, sperm is produced in the testicle and transported to the penis where fluid from the prostate combines with the sperm to produce semen.
Absence of sperm in the ejaculate may be due to 2 primary reasons:
The sperm retrieval techniques help men who were previously considered to be incapable of fathering children as a very few sperm are needed to achieve a successful pregnancy. The ideal technique for harvesting sperm depends on a variety of factors.
Sperm can be retrieved either from;
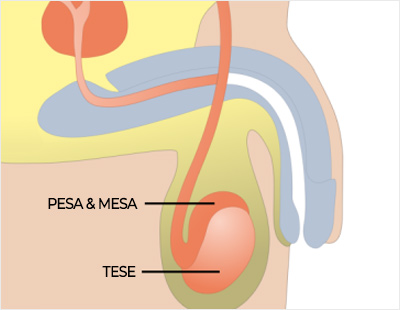
Sperm is retrieved either;
Each approach has certain risks and benefits and each may not be appropriate for everyone. The procedures are performed on the outpatient basis under either local anaesthetic or in a short general anesthesia.
Aspiration of sperm through a needle (TESA, PESA) is the simplest and most cost-effective method. This is routinely performed under local anesthesia and takes approximately 10 minutes.
Harvesting sperm from a man with a testicular problem is much more difficult and often takes several hours. TESE or micro-TESE requires general or spinal anesthesia and an incision on the scrotum to gain access to the testicles.
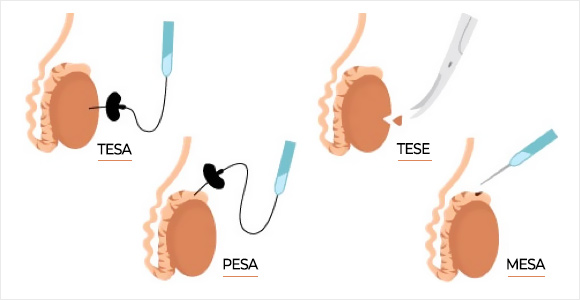
The number of sperm retrieved through these techniques is usually very low compared to the number present in an ejaculate, so the sperm usually need to be used in intra-cytoplasmic sperm injection (IVF-ICSI). Surgically retrieved samples are rarely suitable for use in intrauterine insemination (IUI).
The fresh sperm that is retrieved are immediately used for oocyte fertilization with ICSI method at the same day of oocyte retrieval in an IVF cycle and the spare sperm is cryopreserved to avoid the need to repeat the procedure. If sperm will not be used for ICSI it can be frozen for use at a later time.
PESA and TESA are similar procedures where a needle is used to extract sperm from the epididymis or testicle. PESA and TESA are usually carried out when a man’s ability to naturally release sperm via ejaculation is reduced by blokage of the vas deferens or epididymis. If there is sperm within the epididymis, then PESA will be used, and if not, then TESA will be ideal sperm retrieval option.
The epididymis is an organ that is behind the testicle and is the location where sperm mature and develop the ability to move. The epididymis is an essential component of the male reproductive tract. It is a site of sperm storage and maturation until the time of their discharge to the ductus deferens or vas deferens. Sperm harvested from the epididymis is generally considered better quality than sperm harvested directly from the testicle because they have had more time to mature.
PESA involves collecting sperm via a small needle that is inserted into the epididymis while TESA involves collecting sperm via a fine needle through the skin that is injected directly into the testis and retrieving a small number of the seminiferous tubules themselves. The tubules are then dissected in the laboratory and the contents searched for the presence of sperm.
The benefits of these approaches are that they are relatively painless and do not require an incision in the scrotum or a general anesthetic. Both of these procedures can often be performed with only mild sedation or local anesthetic.
MESA is an open surgical sperm retrieval technique for collecting sperm from epididymis through a small microsurgical skin incision. A surgical microscope is used to open the small tubes within the epididymis to look for sperm.
After anesthesia, the patient's scrotum is stained with an antiseptic solution. Scrotum skin, muscle, and the membranes surrounding the testicle are opened to reveal the testicle and epididymis. The surgeon grasps the testicle firmly with his hand and squeezes the epididymis placed on it with the thumb and index finger.
The epididymis is examined at x 15 x 25 magnification and enlarged intra-testicular canals (tubules) containing golden-yellow, translucent fluid suitable for aspiration is found. Epididymic tubules are exposed with careful incision. Then, the epididymis tubule is entered with an ophthalmic microbisturia. At this point, sperm analysis is performed to decide to continue the process or to complete the procedure.
Epididymis puncture is continued until sufficient fluid is identified microscopically. If sufficient epididymis fluid is identified, it is collected atraumatically with glass micropipettes. Gentle massage of the testicle and epididymis can be applied to increase yield. Several micropipettes are typically used. If no sperm are found, the site is closed with microsuture and another site more closer to the testis is found.
After the procedure is completed the epididymis tubule is sealed with bipolar electrocautery and hemostasis is achieved. The epididymis and testis are placed in their normal positions in the scrotum and the layers are closed with absorbable sutures. A postoperative scrotal support provides patient comfort and prevents edema in the scrotum.
There is no significant difference between the pregnancy rates obtained from the sperm obtained from the testis or epididymis.
The risks of the procedure include bleeding, damage to the epididymis and not being able to obtain sufficient sperm. If these techniques fail, sperm may be found using more advanced methods as TESE or micro-TESE.
The epididymal or testicular fluid is placed onto a petri dish and examined under the inverted microscope (400× magnification) to confirm the presence of motile sperm. The preparation technique to isolate the motile sperm is based on the sperm density and motility and the amount of cellular debris. Patients must be willing to undergo IVF or ICSI after MESA, PESA or TESA.
IVF treatment using PESA, MESA or TESA sperm has a similar success rate to IVF/ICSI using fresh semen produced. Pregnancy rates approach 60% when ICSI is used. Sperm can be used fresh or cryopreserved for future cycles.
I came from abroad for my treatment. Before coming and in the time I spent in Turkey, she was also very supportive. I found her with the suggestion of a friend. She is both helpful and ve...