Conventional In-vitro fertilization (IVF) and ICSI are two common techniques to achieve fertilization. IVF has long been used for treatment of infertility. Although it has made an important role in the treatment of female infertility, it is not an effective treatment in severe male infertility.
Progress in the field of assisted reproduction, and particularly micromanipulation, now heralds a new era in the management of severe male factor infertility, not amenable to medical or surgical correction.
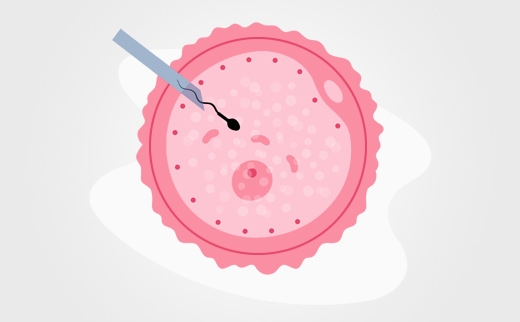
ICSI is the process of injecting a single sperm (or sperm head or nucleus) under a microscope into a one mature egg using a micropipette.
In conventional IVF method following sperm preparation, the oocytes in microdroplets of culture medium in a culture dish, are inseminated with an adequate number of sperm and incubated overnight in the CO2 incubator under ideal temperature and pH conditions. This allows the sperm to penetrate the egg’s zona pellucida (outside shell) and deposit the male’s DNA into the egg’s ooplasm (egg’s cytoplasmic matrix),hopefully resulting in fertilization of the egg.
Fertilization is assessed under a microscope on the next day by the presence of two pronuclei and two polar bodies 16-20 hours post insemination.
It necessitates an optimal sperm number and function to successfully complete the sequence of events leading to fertilization. Conventional IVF failed to solve problems concerning sperm and IVF-ET as treatment for male factor infertility is associated with low fertilization and pregnancy rates than for other indications.
ICSI has been used routinely in many clinics since 1992 for couples with extremely low fertilisation rates with in terms of low sperm count and motility. It leads to a significant fall in cancelled treatments due to fertilisation problems. It does not cause serious problems to children, compared to conventional IVF.
In the ICSI method, sperm used for fertilisation are selected under a microscope which magnifies cells by x400-600. The procedure uses a maximum number of sperm with normal morphology and motility. The first step of the microinjection treatment is to remove cumulus cells which are located around the egg. Then, the egg is fixed using a special tool and the sperm is injected using a thin needle. This process can be done 2-4 hours after harvesting the eggs.
ICSI may be used to alleviate severe male factor infertility due to the lack of sperm in the ejaculate due to severely impaired spermatogenesis (non-obstructive azoospermia) or non-reconstructable reproductive tract obstruction (obstructive azoospermia).
ICSI can be carried out with fresh and frozen-thawed epididymal sperm following microepididymal sperm aspiration (MESA) or testicular sperm following percutaneous sperm aspiration (PESA),testicular sperm extraction (TESE),and modified percutaneous sperm aspiration in patients with obstructive azoospermia (OA),and with testicular sperm in some patients with non-obstructive azoospermia (NOA).
However, not all men having impaired semen parameters are ideal candidates for ICSI for numerous reasons including a lack of addressing the underlying problem causing the male infertility, unknown genetic consequences.
In ICSI the rate of the fertilisation of the eggs is 70%. As a result, a patient with 10 harvested eggs might have up to 7 embryos.
In some patients, the sperm might be morphologically very poor so Intracytoplasmic morphologically selected sperm injection (IMSI) treatment can be applied as a solution.
Thank you very much for everything, Ms. Nilgun. God bless you. You are doing your job properly. We came on advice, we saw everything, quality, service, trust even more than people say....